Most people book a massage when something already hurts. The neck’s been locked up for a week, or the lower back finally gave out, and they figure an hour on a table might help. That’s a fine reason to go. But it’s a limited way to think about what massage actually does and what a consistent bodywork practice can offer over time.
This isn’t about selling you on wellness. It’s about what the evidence shows and why more people, including those managing anxiety, chronic pain, or burnout, are building massage and somatic therapies into their regular routines rather than treating them as occasional fixes.
What Happens to the Body During a Session
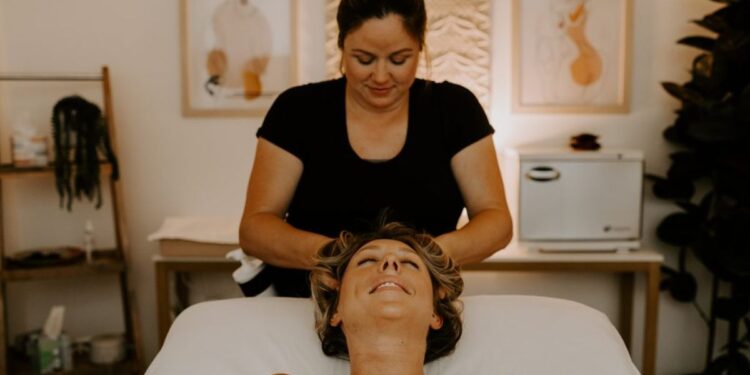
Touch affects the nervous system in specific, measurable ways. When skilled pressure is applied to muscle tissue, the body shifts away from sympathetic activation, the state associated with stress and threat response, and moves toward parasympathetic dominance. Cortisol drops. Serotonin and dopamine increase.
Research has shown that massage can reduce symptoms of anxiety and depression in both clinical and non-clinical populations and that it may help regulate the autonomic nervous system in ways that support mood and emotional stability. That’s not a minor finding. For someone carrying chronic stress, those physiological shifts have real clinical relevance.
At the tissue level, massage may improve perceived stiffness and mobility, support local circulation, and help reduce the kind of low-grade physical tension that builds up from sedentary work or repetitive strain. Most people notice something after a single session. The longer-term benefits take consistency.
The Mental Health Connection
This is where massage tends to get undersold.
The National Center for Complementary and Integrative Health has reviewed research on massage across a range of conditions, including anxiety, depression, and chronic pain, with findings that support its role as a meaningful complement to conventional care. That level of documented interest from a federal health agency reflects how much the clinical conversation has changed over the past two decades.
No credible practitioner would argue that massage replaces therapy or medication. But as part of a broader care plan, it offers something genuinely hard to find elsewhere: a structured, safe, somatic experience that helps the body come down from chronic activation. For people who carry stress physically, in tight shoulders, a clenched jaw, or a neck that won’t release, that kind of release has value.
A study referenced by the National Institutes of Health found that massage therapy is frequently used alongside conventional treatment by people managing anxiety and depression and that its documented effects on cortisol, serotonin, and dopamine suggest a credible mechanism beyond simple relaxation. For people in recovery from addiction or trauma, where the body-mind relationship is often central to healing, addressing physical tension directly is increasingly recognized as a legitimate piece of integrative care.
A Note on Float Therapy
Float tanks, also called sensory deprivation tanks or REST (restricted environmental stimulation therapy), work through a different but complementary mechanism. You’re floating in a shallow pool of warm, heavily salted water in near-total silence and darkness. The body becomes essentially weightless. Without external sensory input, the nervous system has nowhere to go except down.
The research on floatation is still developing, but early findings are promising, particularly around anxiety reduction, pain perception, and sleep quality. Some people find it easier to access a genuinely relaxed state in a float tank than through any other method. Others use it to decompress after intense physical training. Either way, it pairs well with massage; one addresses the soft tissue and nervous system through direct contact, and the other through the removal of stimulation entirely.
In clinics that offer both, it’s practical to combine them in a single visit, which tends to compound the effects.
Pain Management
Chronic pain rarely exists in isolation. Depression and anxiety frequently show up alongside persistent pain, and each one can make the other harder to manage. Massage doesn’t resolve that complexity, but it addresses more than one layer of it at a time.
There’s solid evidence that massage is particularly useful for musculoskeletal pain, including lower back pain, neck stiffness, and tension headaches. Some techniques used in clinical settings, including instrument-assisted soft tissue work and gua sha therapy, have been studied in populations dealing with chronic conditions. Gua sha has roots in traditional Chinese medicine and involves controlled pressure applied with a smooth tool along the skin’s surface. Research suggests it may support circulation and reduce perceived muscle tension, though the evidence base is still growing and findings vary across populations and conditions.
Sleep is worth mentioning separately here. Most people with chronic pain also have disrupted sleep. Massage has been shown to support sleep quality, likely through its effects on the nervous system. Better sleep makes pain more manageable, improves emotional regulation, and supports recovery in general. The benefits tend to stack.
What a Session Actually Feels Like
Clinical language can make this all sound more sterile than it is. A good massage session, one where the therapist has taken a health history, asked about problem areas, and is actually paying attention, feels like sustained, intelligent pressure. Not painful, not performative. Just deliberate contact that works through tension instead of around it.
Float therapy feels like nothing, which is the point. The first few minutes can feel strange. The mind wants something to respond to. Once that passes, most people describe a kind of quiet that’s hard to find anywhere else. An hour in a float tank often feels longer in the best possible way.
Neither experience requires anything from you except showing up. That’s part of why they work for people who are exhausted or overstimulated. The session does the work.
Building It Into a Routine
The shift worth making is treating self-care as infrastructure rather than reward. Massage, float therapy, breathwork, movement, these aren’t things you earn after a hard month. They’re practices that, used consistently, build the kind of nervous system resilience that makes hard months more manageable.
The practical barrier for most people is cost and access. That’s fair. Many providers now offer membership structures, shorter session formats, or bundled options that make regular visits more realistic than a one-off appointment. If you’re managing anxiety, chronic pain, or burnout, a standing monthly session is almost certainly more useful than a single visit every six months when things get bad.
When to Check With a Doctor First
Massage is safe for most people, but a few situations call for medical clearance beforehand. Anyone with a clotting disorder, recent surgery, certain skin conditions, or specific cardiovascular concerns should talk to their doctor before booking. A qualified therapist will always take a health history before starting and should ask about medications or conditions that might affect technique choices.
As integrative approaches to health continue to gain clinical traction, massage and somatic therapies are being taken more seriously, not as alternatives to conventional care, but as modalities that address the body as part of the whole picture. That’s a reasonable way to think about them. And it’s why more people are making room for this kind of care in their regular routines rather than waiting until they have no choice.